Research
Preclinical Theranostics
Our research focuses on theranostics with the goal to deliver new insights into tumor biology, heterogeneity and metabolism, and their relationship and relevance to functional imaging and biomarker-driven treatments in nuclear medicine.
What are theranostics?
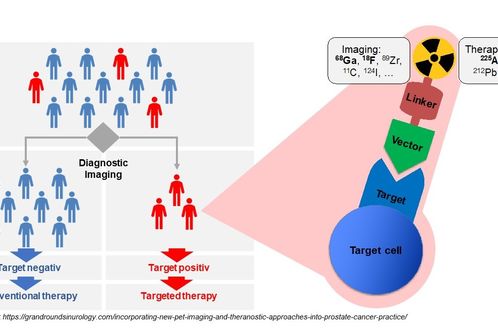
The term theranostics combines the words diagnosis and therapy; it represents a precision medicine approach relying on a specific targeted diagnostic test that helps to select patients for a specific targeted therapy. In nuclear medicine, radioligands are used for theranostics. Radioligands are radio-labelled molecules that bind to a cell surface receptor on target cells. When coupled to radio-isotopes like Gallium-68 or Fluor-18, radioligands can be used for imaging with positron emission tomography (PET), single-photon emission computed tomography (SPECT), or scintigraphy. This imaging facilitates the selection of patients for subsequent radioligand therapy. Radioligand therapy is an emerging treatment modality for various cancers. In radioligand therapy, the same or a very similar radioligand as that used for imaging is coupled to a therapeutic radioisotope (e.g., Actinium-225, Lutetium-177, Yttrium-90) to deliver ionizing radiation specifically to tumors. Radioligand therapy can thus be described as a type of targeted, systemic radiotherapy. In contrast to conventional radiotherapy, radioligand therapies are systemically administered, and radioligands are internalized upon binding to tumor cells. As a consequence, metastases throughout the body can be targeted, and tumors are irradiated for hours to days.
Figure 1. Theranostics. In theranostics, patients are first screened for presence of a specific characteristic using diagnostic imaging. Patients who express the target can be treated with a targeted therapy. Thus, theranostics allow individualization of therapeutic regimen. In nuclear medicine, the key tools of theranostics are radioligands. Radioligands are radio-labeled molecules that bind to a specific target. Target expression can be visualized and anatomically localized by detecting the radioactive signal from radioligands that have bound to their target (e.g., by PET/CT). When radioligands are coupled to therapeutic radioisotopes they can be used for radioligand therapy, a type of targeted, systemic radiotherapy. Radioligand therapy delivers ionizing radiation specifically to all target-positive cells (e.g., tumor cells) in the body, leading to the death of these cells.
Characterizing phenotypic imaging biomarkers
Molecular imaging in nuclear medicine combines imaging modalities like PET and SPECT with computed tomography (CT) or magnet resonance tomography to derive detailed information on disease. In the clinic, molecular imaging is mainly used for diagnosis, staging, monitoring response to therapy (e.g., by pre- and post-therapeutic FDG-PET/CT), and to select patients for RLT (e.g., PSMA-PET/CT). Our group aims at establishing molecular imaging as a phenotypic biomarker, i.e., to connect imaging information with the tumor biology, metabolism and intra- and inter-individual tumor heterogeneity. Ultimately, this will provide imaging strategies that can guide selection of individualized - and therefore more effective and less toxic - treatment regimens that improve quality of life and overall survival of patients.
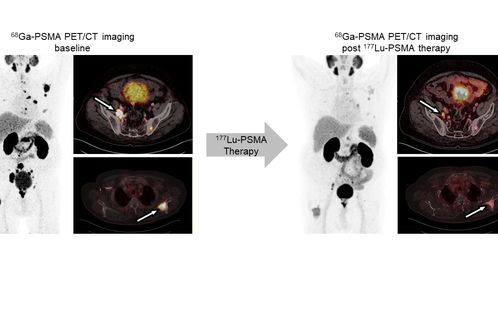
Figure 2. Illustrated example of imaging biomarker use in theranostics. PET/CT using the radioligand 68Ga-PSMA visualizes expression of the prostate-specific membrane antigen (PSMA). Diagnostic imaging: 68Ga-PSMA PET/CT detected prostate cancer metastases. Imaging to select patients and therapy planning: Intense enrichment of 68Ga-PSMA indicated high PSMA expression levels on tumor lesions rendering the patient eligible for treatment with 177Lu-PSMA radioligand therapy. Monitoring therapeutic response: Comparison of baseline and post radioligand therapy PET/CT images suggested partial response. Phenotypic biomarker: The exact conclusions about disease pathology that can be derived from an image often remain ambiguous. Establishing phenotypic imaging biomarkers that gives detailed information on underlying biology, metabolism and heterogeneity of target expression is highly warranted to improve patient care and outcome. (Images: courtesy of University Hospital Essen, Clinic for Nuclear Medicine)
Elucidate and overcome resistance to radioligand therapy
Radioligand therapy is a promising yet rarely curative oncological treatment option. Our research aims at identifying predictors (biomarkers) for and determinants (molecular and cellular processes) of response/non-response to radioligand therapy. We investigate tumor cell intrinsic resistance mechanisms, tumor protection by microenvironmental factors (immunosuppression, stroma), and suboptimal tumor radiation dose delivery using cancer models and patient samples, and diverse in vitro, ex vivo and in vivo analyses. We use the knowledge gained from these studies to rationally design and provide proof-of-principle for new radioligand therapy combination regimens that can be translated into the clinic.
Experimental Radiochemistry: Implement new approaches in nuclear oncology
Building on the first success stories of theranostics, we evaluate oncological targets and develop organic chemical or radiochemical processes for the production and development of new radioligands for imaging and therapy. This includes the design, chemical synthesis, radiolabeling, and in vitro, in vivo, and ex vivo evaluation of ligands.
Preclinical nuclear cardiology
The role of molecular imaging technologies in detecting, evaluating, and monitoring cardiovascular disease and their treatment is expanding rapidly. Gradually replacing the conventional anatomical or physiological approaches, molecular imaging strategies using biologically targeted markers provide unique insight into pathobiological processes at molecular and cellular levels and allow for cardiovascular disease evaluation and individualized therapy. We use SPECT and PET imaging to assess myocardial perfusion to find areas of damaged heart muscle and visualize the size and location of myocardial infarction. Specific radiotracers are used to assess cardiac inflammation and fibroblast activity in different cardiac disease models.